Diabetes and Macular Degeneration are more treatable than ever.
MACULAR DEGENERATION
PREFACE: The future of macular degeneration treatment is exceptionally optimistic. In fact, retinal research into improving efficacy, reducing treatment burden, and even curing the disease via new therapies is leading the way in the entire medical field. This category of research will translate to advancements in the treatment of retinal disease and a number of other general medical disorders.
LATEST AVAILABLE AND UPCOMING TREATMENTS:
- Vabysmo (Faricimab)
- Syfovre (Pegcetacoplan)
- Susvimo (Ranibizumab ocular implant)
- Eylea (Aflibercept)
- Avastin (Bevacizumab)
As the name suggests, macular degeneration involves a degeneration of tissues under the retina. The most common form of macular degeneration is age-related macular degeneration, most prevalent in the population aged 60 and older. Age-related macular degeneration is also most prevalent in Caucasians. It is particularly detrimental to quality of life because it preferentially affects the central vision. For this same reason, its only saving grace is that it will never completely blind a person in that it spares the peripheral vision. With this peripheral vision a person can be reasonably expected to get around, although at its worst macular degeneration will take our ability to read, drive, use a computer, or even recognize faces.
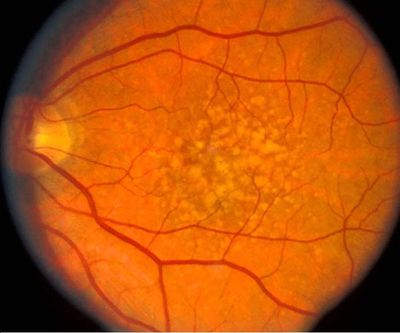
There are two main categories of macular degeneration, dry and wet. Ninety percent of macular degeneration is the dry form which involves a degeneration of the tissues under the retina, and ultimately the retina itself. This form is the earlier and less aggressive form of the disease. It should be understood, however, that dry macular degeneration alone can result in extreme vision loss. The earliest component of dry macular degeneration is the accumulation of deposits, called drusen, under the retina. These drusen can be visible on retinal examination and their concentration and size correlate with the severity of the disease. More advanced forms of dry macular degeneration involve entire patches of degeneration in and under the retina, visible on examination as what is called geographic atrophy. As stated above, although still a dry form of macular degeneration, this can result in markedly reduced vision.
Dry macular degeneration cannot currently be reversed by medical intervention, but to a significant degree, its progression can be slowed or abated with a number of interventions. These include the regular use of eye vitamins which include the minerals and vitamins studied in the Age Related Eye Disease Study or AREDS. Currently the AREDS 2 formula of vitamins and minerals is recommended. Injectables such as Syfovre have been developed for dry macular degeneration.
Another important intervention is cessation of smoking, which is an independent risk factor for the progression of macular degeneration to the wet or more aggressive form. Hypertension, or high blood pressure, is still another independent risk factor for the development of wet macular degeneration. Studies show less than half of Americans with hypertension have their blood pressure under control, and in practice this correlates directly with worsening macular degeneration in patients. There is almost never a reason that high blood pressure cannot be controlled, and most often it can be controlled by simply adjusting the dose of anti-hypertensive medications, resulting in a much better chance of maintenance of vision in age-related macular degeneration.
Wet macular degeneration is a more aggressive form of the disease and responsible for most of the vision loss associated with macular degeneration. Approximately 10 to 15% of eyes suffering dry macular degeneration will progress to this more aggressive form. The disease mechanisms involved in wet macular degeneration involve the tissues adjacent to the retina and include increased inflammation, leakage of blood vessels, degeneration of vital tissues, and eventually the growth of new unhealthy blood vessels under the retina. These new blood vessels unfortunately develop most often beneath the macula, which is the part of the retina responsible for fine central vision. It is for this reason the typical vision loss in macular degeneration affects the central and not the peripheral vision. These new unhealthy blood vessels are prone to leakage of fluid and frank bleeding which can lead to scar tissue and further degeneration of the retina if untreated.
In past years, no good treatments for wet macular degeneration existed. Both patients and their retinal specialists could only watch in frustration as precious sight was lost permanently over time. Eventually hot lasers were used with some success, but often with residual vision loss caused by the laser as well as the disease. Photodynamic therapy, or cold laser, eventually allowed for less residual damage and served as an effective treatment for certain lesions. This cold laser, however, still left over half of treated eyes with a loss of vision over time.
In more recent years, steroids and newer medications including VEGF inhibitors have been used more successfully to limit both the leakage and growth of the unhealthy blood vessels developing in wet macular degeneration. Combinations of these and past treatments are being used with more success than previously could be offered to patients with macular degeneration. The most commonly used class of drugs is VEGF-inhibitors. Included in this group are the drugs avastin, Lucentis, and Eylea which have allowed approximately 90% of macular degeneration patients, receiving early treatment, to maintain or gain vision. Many new treatments are in constant research, but no treatment can substitute for regular examination and early diagnosis.
Interventions such as the use of AREDS 2 supplements, cessation of smoking, aggressive control of blood pressure, diet high in vegetables and low in fats, control of cholesterol, treatment of sleep apnea, and even control of major anxiety can benefit patients with macular degeneration
Articles
FDA Approves Beovu
FDA Approves Beovu (brolucizumab-dbll) for the Treatment of Wet Age-Related Macular Degeneration (AMD)
EAST HANOVER, N.J., Oct. 8, 2019 /PRNewswire/ -- Novartis today announced that the U.S. Food and Drug Administration (FDA) approved Beovu (brolucizumab-dbll) injection, also known as RTH258, for the treatment of wet age-related macular degeneration (AMD)1. Beovu is the first FDA-approved anti-VEGF to offer both greater fluid resolution versus aflibercept and the ability to maintain eligible wet AMD patients on a three-month dosing interval immediately after a three-month loading phase1 with uncompromised efficacy.
"Beovu meets our goals in clinical practice for treating wet AMD: improving vision and drying retinal fluid," said Dr. Pravin U. Dugel, Managing Partner, Retinal Consultants of Arizona; Clinical Professor, Roski Eye Institute, Keck School of Medicine, University of Southern California; and principal investigator of the HAWK clinical trial. "With Beovu, greater fluid reduction was demonstrated through larger decreases in retinal thickness and a higher proportion of patients with drier retinas. Coupled with the potential to treat patients with quarterly injections, this approval may change the way we approach the treatment of wet AMD."
The approval of Beovu was based on findings from the Phase III HAWK and HARRIER clinical trials, in which Beovu demonstrated non-inferiority versus aflibercept in mean change in best-corrected visual acuity (BCVA) at year one (week 48)1,2. In both clinical trials, approximately 30% of patients gained at least 15 letters at year one1,2. In HAWK and HARRIER, BEOVU showed greater reduction in central subfield thickness (CST) as early as week 16 and at year one, and fewer patients had intra-retinal (IRF) and/or sub-retinal fluid (SRF)2. Retinal fluid is a key marker of disease activity6.
Wet AMD is a chronic, degenerative eye disease caused by an excess of VEGF, a protein that promotes the growth of abnormal blood vessels underneath the macula, the area of the retina responsible for sharp, central vision7,8. Fluid that leaks out of these abnormal blood vessels disrupts the normal retinal structure and ultimately damages the macula8-10. The Beovu molecule is engineered to deliver the highest concentration of drug, providing more active binding agents than other anti-VEGFs2. By inhibiting VEGF, Beovu suppresses the growth of abnormal blood vessels and the potential for fluid leakage into the retina2.
"The approval of Beovu delivers on the Novartis commitment to reimagining treatments for patients suffering from serious visual impairment," said Marie-France Tschudin, President, Novartis Pharmaceuticals. "The product labels of existing treatments state that they are not as effective when dosed every 12 weeks. Beovu is the first to offer less frequent dosing in the first year of therapy while maintaining its effectiveness. This gives more time for wet AMD patients to focus on what's important in their lives."
In HAWK and HARRIER, eligible patients could be maintained on a three-month dosing interval immediately after the loading phase1,2. At year one, over half of patients were maintained on the three-month dosing interval (56% in HAWK and 51% in HARRIER)1,2. The remaining patients in the study were treated on a two-month dosing schedule1,2.
Beovu exhibited an overall safety profile comparable to aflibercept. Beovu is contraindicated in patients with ocular or periocular infections, active intraocular inflammation or with known hypersensitivity to brolucizumab or any of the excipients in Beovu1. Hypersensitivity reactions may manifest as rash, pruritus, urticaria, erythema or severe intraocular inflammation1.
The most common adverse events (≥5% of patients) with Beovu were vision blurred, cataract, conjunctival hemorrhage, vitreous floaters and eye pain1,2.
Wet AMD distorts central vision and ultimately causes blindness and loss of independence11,12. Estimates suggest that in 2020, 1.75 million people in the U.S. will be living with wet AMD13-15, making it a growing public health concern. Early symptoms of wet AMD include blurry or wavy vision8. As the disease progresses, patients lose central vision so it becomes difficult to see objects directly in front of them8.
"As sight disappears, so does a person's connection to the world," said Dawn Prall, Founder and Executive Director, The Support Sight Foundation. "We welcome a new treatment that helps maintain vision and has the potential for quarterly treatments, which can reduce the burden on patients and their caregivers and help people with wet AMD keep doing what they love with the people they love."
With this approval, Novartis is offering Beovu Your Way™ in the U.S. This program provides personalized, one-on-one support for patients and caregivers, with access to a care specialist committed to understanding patients' unique needs and preferences. Novartis is proud to be partnering with patient advocacy organizations to deliver educational materials for patients and caregivers, with the goal of empowering wet AMD patients to live safely and independently.
About Beovu (brolucizumab-dbll)
Beovu (brolucizumab-dbll) is the most clinically advanced humanized single-chain antibody fragment (scFv)2,16. Single-chain antibody fragments are highly sought after in drug development due to their small size, enhanced tissue penetration, rapid clearance from systemic circulation and drug delivery characteristics16-18.
The proprietary innovative structure results in a small molecule (26 kDa) with potent inhibition of, and high affinity to, all VEGF-A isoforms17. Beovu is engineered to deliver the highest concentration of drug, providing more active binding agents than other anti-VEGFs2,16. In preclinical studies, Beovu inhibited activation of VEGF receptors through prevention of the ligand-receptor interaction17-19. Increased signaling through the VEGF pathway is associated with pathologic ocular angiogenesis and retinal edema20. Inhibition of the VEGF pathway has been shown to inhibit the growth of neovascular lesions and suppress endothelial cell proliferation and vascular permeability20.
About the HAWK and HARRIER studies
With more than 1,800 patients across nearly 400 centers worldwide, HAWK (NCT02307682) and HARRIER (NCT02434328) are the first and only global head-to-head trials in patients with wet AMD that prospectively demonstrated efficacy at week 48 using an innovative q12w/q8w regimen, with a majority of patients on q12w immediately following the loading phase2. Both studies are 96-week prospective, randomized, double-masked multi-center studies and part of the Phase III clinical development of BEOVU2. The studies were designed to compare the efficacy and safety of intravitreal injections of brolucizumab 6 mg (HAWK and HARRIER) and 3 mg (HAWK only) versus aflibercept 2 mg in patients with wet AMD2.
About Wet Age-Related Macular Degeneration
Wet AMD is a leading cause of severe vision loss and legal blindness in people over the age of 65 in North America, Europe, Australia and Asia, impacting an estimated 20 million people worldwide4,5,11. It is estimated that 1.75 million people in the U.S. will be living with wet AMD in 202013-15. Wet AMD occurs when abnormal blood vessels form underneath the macula, the area of the retina responsible for sharp, central vision8-10. These blood vessels are fragile and leak fluid, disrupting the normal retinal architecture and ultimately causing damage to the macula8-10.
Early symptoms of wet AMD include distorted vision (or metamorphopsia) and difficulties seeing objects clearly8,21. Prompt diagnosis and intervention are essential10. As the disease progresses, cell damage increases, further reducing vision quality8. This progression can lead to a complete loss of central vision, leaving the patient unable to read, drive or recognize familiar faces and potentially depriving them of their independence8,12. Without treatment, vision can rapidly deteriorate22.
- BEOVU [prescribing information] East Hanover, NJ. Novartis: 2019.
- Dugel P, et al. HAWK and HARRIER: Phase 3, multicenter, randomized, double-masked trials of brolucizumab for neovascular age-related macular degeneration [published online ahead of print]. Ophthalmology. 2019.
- Varano M, et al. Current barriers to treatment for wet age-related macular degeneration (wAMD): findings from the wAMD patient and caregiver survey. Clin Ophthalmol. 2015;9:2243–2250.
- Wong WL, Su X, Li X, et al. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: a systematic review and met analysis. Lancet Glob Health. 2014;2:106-16.
- Singer M. Advances in the management of macular degeneration. F1000Prime Rep. 2014;6:29.
- Arnold J, et al. The role of sub-retinal fluid in determining treatment outcomes in patients with neovascular age-related macular degeneration--a phase IV randomised clinical trial with ranibizumab: the FLUID study. BMC Ophthalmol. 2016;143(4):679-680.
- Qazi Y, et al. Mediators of ocular angiogenesis. J. Genet. 2009;88(4):495-515.
- National Eye Institute. Facts About Age-Related Macular Degeneration. Available at https://nei.nih.gov/health/maculardegen/armd_facts (link is external). Accessed September 2019.
- World Health Organization. Priority eye diseases: Age-related macular degeneration. Available at http://www.who.int/blindness/causes/priority/en/index7.html (link is external). Accessed September 2019.
- NHS Choices. Macular Degeneration. Available at http://www.nhs.uk/Conditions/Macular-degeneration/Pages/Introduction.aspx (link is external). Accessed September 2019.
- Schmidt-Erfurth U, et al. Guidelines for the management of neovascular age-related macular degeneration by the European Society of Retina Specialists (EURETINA). Br J Ophthalmol. 2014;98:1144-1167.
- Mitchell J, Bradley C. Quality of life in age-related macular degeneration: a review of the literature. Health Qual Life Outcomes. 2006;4:97.
- Friedman DS, O'Colmain BJ, Munoz B, et al. Prevalence of age-related macular degeneration in the United States. Arch Ophthalmol. 2004;122(4):564-72.
- Klein R, Chou CF, Klein BE, Zhang X, Meuer SM, Saaddine JB. Prevalence of age-related macular degeneration in the U.S. population. Arch Ophthalmol. 2011;129(1):75-80.
- American Academy of Ophthalmology. Age-related macular degeneration preferred practice patterns. Available at: https://www.aao.org/preferred-practice-pattern/age-related-macular-degeneration-ppp-2015 (link is external). Accessed September 2019.
- Nimz EL, et al. Intraocular and systemic pharmacokinetics of brolucizumab (RTH258) in nonhuman primates. The Association for Research in Vision and Ophthalmology (ARVO) annual meeting. 2016. Abstract 4996.
- Escher D, et al. Single-chain antibody fragments in ophthalmology. Oral presentation at EURETINA congress. 2015. Abstract.
- Gaudreault J, et al. Preclinical pharmacology and safety of ESBA1008, a single-chain antibody fragment, investigated as potential treatment for age related macular degeneration. ARVO Annual Meeting abstract. Invest Ophthalmol Vis Sci. 2012;53:3025. http://iovs.arvojournals.org/article.aspx?articleid=2354604 (link is external). Accessed September 2019.
- Tietz J, et al. Affinity and Potency of RTH258 (ESBA1008), a Novel Inhibitor of Vascular Endothelial Growth Factor A for the Treatment of Retinal Disorders. IOVS. 2015; 56(7):1501.
- Kim R. Introduction, mechanism of action and rationale for anti-vascular endothelial growth factor drugs in age-related macular degeneration. Indian J Ophthalmol. 2007;55(6):413-415.
- Healthline. What is metamorphopsia? Available at https://www.healthline.com/health/metamorphopsia (link is external). Accessed September 2019.
- van Lookeren Campagne M, et al. Mechanisms of age-related macular degeneration and therapeutic opportunities. J Pathol. 2014; 232(2):151-64. doi: 10.1002/path.4266.
Source: Novartis
Posted: October 2019
Alkahest Announces Positive Top-Line Data from Two Phase 2a Studies of AKST4290 in Individuals with Wet Age-Related Macular Degeneration
Both treatment naïve and treatment refractory individuals experienced improved visual acuity
SAN CARLOS, Calif., — Alkahest Inc., a clinical-stage biotechnology company focused on developing transformative therapies to treat age-related diseases, today announced top-line data from two Phase 2 studies of AKST4290 (formerly ALK4290) for the treatment of wet age-related macular degeneration (wAMD). AKST4290 was found to be safe and well tolerated, with gains in visual acuity for both treatment naïve and treatment refractory patient groups.
“Current treatments for wAMD involve regular intravitreal injections of anti-VEGF therapies, which can be costly and present adherence challenges. These challenges often result in undertreatment,” said Jonas Hannestad, M.D. Ph.D., Vice President of Clinical Development at Alkahest. “These early results demonstrate the feasibility of using an oral agent to provide a conveniently administered treatment option for patients suffering from wAMD. We look forward to providing additional data from these studies at upcoming medical conferences and pursuing additional trials to confirm these results.”
The AKST4290-201 study is a Phase 2a clinical trial designed to evaluate the therapeutic effects and safety of a six-week oral treatment regimen of AKST4290 in patients with newly diagnosed wAMD who are naïve to any treatment. The AKST4290-202 study is a parallel Phase 2a clinical trial designed to evaluate the therapeutic effects and safety of the same treatment regimen in patients with refractory wet AMD no longer responding to anti-VEGF therapy. The majority of patients across both studies experienced improvement in best-corrected visual acuity (BCVA), and there were no severe or serious adverse events reported.
About AKST4290
AKST4290 is an orally administered CCR3 inhibitor that blocks the action of eotaxin, an immunomodulatory protein that increases as humans age. By targeting eotaxin and its downstream effects, AKST4290 may slow the hallmark inflammation and neovascularization of wet AMD and other age-related diseases. Alkahest acquired AKST4290 from Boehringer-Ingelheim and has exclusive rights for development and commercialization worldwide.
About Alkahest
Alkahest is a clinical stage biopharmaceutical company dedicated to treating neurodegenerative and age-related diseases with transformative therapies targeting the aging plasma proteome. The Alkahest pipeline includes multiple therapeutic candidates ranging from selected plasma fractions to protein-targeted interventions, which aim to slow the detrimental biological processes of aging. Alkahest is developing novel plasma-based therapies in collaboration with Barcelona, Spain-based Grifols, a global healthcare company and leading producer of plasma therapeutics.
https://www.alkahest.com/news/latest-news/
Patients with macular degeneration show improvement with high-dose statin treatment
Date:February 4, 2016Source:Massachusetts Eye and Ear InfirmarySummary:A phase I/II clinical trial has found that some patients taking high doses of atorvastatin (cholesterol-lowering medication) had complete resolution of lipid deposits in the dry form of age-related macular degeneration. AMD is the leading cause of blindness in the developed world, and though effective treatments are available for the wet AMD, they are currently lacking for the more-prevalent dry form.Share: FULL STORY
Researchers at Massachusetts Eye and Ear/Harvard Medical School and the University of Crete have conducted a phase I/II clinical trial investigating the efficacy of statins (cholesterol-lowering medications) for the treatment of patients with the dry form of age-related macular degeneration (AMD) -- the leading cause of blindness in the developed world.
Although effective treatments are available for the wet form of AMD, they are currently lacking for the more prevalent dry form. The researchers found evidence that treatment with high-dose atorvastatin (80mg) is associated with regression of lipid deposits and improvement in visual acuity, without progression to advanced disease, in high-risk AMD patients. Their findings were published in EBioMedicine--a new online journal led by editors of the journals Cell and The Lancet--and not only further the connection between lipids, AMD and atherosclerosis, but also present a potential therapy for some patients with dry AMD.
"We found that intensive doses of statins carry the potential for clearing up the lipid debris that can lead to vision impairment in a subset of patients with macular degeneration," said Joan W. Miller, M.D., the Henry Willard Williams Professor and Chair of Ophthalmology at Harvard Medical School and Chief of Ophthalmology at Massachusetts Eye and Ear and Massachusetts General Hospital. "We hope that this promising preliminary clinical trial will be the foundation for an effective treatment for millions of patients afflicted with AMD."
Affecting more than 150 million patients worldwide, AMD is associated with an accumulation of drusen (deposits of lipid and fatty proteins) under the retina, and patients with AMD experience blurred vision or blindness in the center of the visual field. There are two forms of AMD: "wet" and "dry." The wet form accounts for approximately 15 percent of AMD cases and is treated using therapies previously developed at Mass. Eye and Ear/Harvard Medical School. The "dry" form is more common, accounting for approximately 85 percent of cases, and effective therapies are currently lacking.
Ophthalmologists and vision researchers have long suspected that there may be a connection between dry AMD and atherosclerosis. In dry AMD, physicians often see soft, lipid-rich drusen in the outer retina, similar to the build-up of lipid material in the inner walls of blood vessels in atherosclerosis. Statin use is widespread in middle-aged and older individuals, who also have an increased risk of AMD; however, previous studies have shown very little correlation between regular statin use and improvements in AMD. The authors of the EBioMedicine paper hypothesized that, due to the heterogeneous nature of the disease, patients with soft, lipid-rich drusen may respond better to statins prescribed at higher dosages.
"Not all cases of dry AMD are the exactly the same, and our findings suggest that if statins are going to help, they will be most effective when prescribed at high dosages in patients with an accumulation of soft, lipid material" said Demetrios Vavvas, M.D., Ph.D., a clinician scientist at Mass. Eye and Ear and Co-Director of the Ocular Regenerative Medicine Institute at Harvard Medical School. "These data suggest that it may be possible to eventually have a treatment that not only arrests the disease but also reverses its damage and improves the visual acuity in some patients."
Twenty-three patients with dry AMD marked by soft lipid deposits in the outer retina were prescribed a high dose (80mg) of atorvastatin, the generic name of the statin marketed as Lipitor® and several generic equivalents. Of the 23 patients, 10 experienced an elimination of the deposits under the retina and mild improvement in visual acuity. Other techniques that have attempted to eliminate the deposits have mostly failed with the disease continuing to progress to more advanced dry AMD or a conversion to the wet form of AMD.
As the next step for this line of research, the investigators plan to expand to a larger prospective multicenter trial to further investigate the efficacy of the treatment in a larger sample of patients with dry AMD.
"This is a very accessible, FDA-approved drug that we have tremendous experience with," said Dr. Vavvas. "Millions of patients take it for high cholesterol and heart disease, and based on our early results, we believe it offers the potential to halt progression of this disease, but possibly even to restore function in some patients with dry AMD."
This work was supported by the Yeatts Family Foundation, the Loefflers Family Foundation and the Research to Prevent Blindness Foundation.
Authors on the EBioMedicine paper include senior author Joan W. Miller, M.D., FARVO, first author Demetrios G. Vavvas, M.D., Ph.D., Anthony B. Daniels, M.D., John I. Loewenstein, M.D., Lucy H. Young, M.D., Ph.D., Evangelos S. Gragoudas, M.D., Dean Eliott, M.D., and Ivana K. Kim, M.D., of the Department of Ophthalmology at Mass. Eye and Ear/Harvard Medical School, Jeremy W. Goldfarb, M.D., of the Department of Anesthesiology at Mass. Eye and Ear/Harvard Medical School, and Zoi G. Kapsala, M.D., Emmanuel Ganotakis, M.D., and Miltiadis K. Tsilimbaris, M.D., Ph.D. of the Department of Ophthalmology at the University of Crete in Greece.
Story Source:
Materials provided by Massachusetts Eye and Ear Infirmary. Note: Content may be edited for style and length.
Journal Reference:
- Demetrios G. Vavvas, Anthony B. Daniels, Zoi G. Kapsala, Jeremy W. Goldfarb, Emmanuel Ganotakis, John I. Loewenstein, Lucy H. Young, Evangelos S. Gragoudas, Dean Eliott, Ivana K. Kim, Miltiadis K. Tsilimbaris, Joan W. Miller. Regression of some High-Risk Features of Age-Related Macular Degeneration (AMD) in Patients Receiving Intensive Statin Treatment. EBioMedicine, 2016; DOI: 10.1016/j.ebiom.2016.01.033

Reviews
Retinitis Pigmentosa & Stargardt
Patient Portal

Subscribe
Contact Us
Please send us a message or call us for an appointment.
We are located conveniently at I-10 and N. Causeway Blvd. near Lakeside Mall.
THE RETINA INSTITUTE, New Orleans, LA
2701 North Causeway Boulevard, Metairie, Louisiana 70002, United States
Hours
Open today | 08:00 am – 04:30 pm |
8am - 4:30pm Monday through Friday
Closed Saturday and Sunday
Copyright © 2005-2024 The Retina Institute — All Rights Reserved.
Most insurance accepted. Care Credit available.
- HOME
- NEW PATIENTS / REVIEWS
- DR. EBRAHIM
- STORE
- CAREERS
- PORTAL & PAYMENT
- AMSLER GRID
- VIDEO GALLERY
- RESEARCH
- GENETICS
- ACUTE RETINAL NECROSIS
- AUTOIMMUNE RETINOPATHY
- BIRDSHOT CHORIORETINITIS
- CANCER ASSOC. RETINOPATHY
- CENTRAL SEROUS/POLYPOIDAL
- COATS' DISEASE
- CONE ROD DYSTROPHY
- CYTOMEGALOVIRUS RETINITIS
- DIABETIC RETINOPATHY
- ENDOPHTHALMITIS
- EPIRETINAL MEMBRANE
- FLOATERS
- HIGH BLOOD PRESSURE
- HISTOPLASMOSIS
- HIV RETINOPATHY
- LATTICE DEGENERATION
- MACULAR DEGENERATION
- MACULAR HOLE
- MELANOMA
- METASTASES
- MYELINATED RETINAL NFL
- OCULAR ISCHEMIC SYNDROME
- OPEN GLOBE INJURY
- OPTIC NERVE HEAD DRUSEN
- PROLIF. VITREORETINOPATHY
- RETINAL ARTERY OCCLUSION
- RETINAL DETACHMENT
- RETINAL DYSTROPHIES
- RETINAL VEIN OCCLUSION
- RETINITIS PIGMENTOSA
- RETINOSCHISIS
- SARCOIDOSIS
- SICKLE CELL RETINOPATHY
- STARGARDT DISEASE
- TOXOPLASMIC CHOROIDITIS
- UVEITIS
- VITREOUS DETACHMENT
- VITREOUS HEMORRHAGE
- WHITE DOT SYNDROMES
